Insights from Our Inspections: Key Themes in GP Practices
Following our assurance work in 2024-25, we inspected 30 GP practices and reported on a number of issues across Wales. In some circumstances we have needed to ask the practices to take immediate action to reduce risks to patient safety.

We acknowledge that GP practices remain under significant pressure, due to unprecedented demand on their services and other strains on the wider NHS. This pressure has been reflected in our findings, which have varied.
Despite this variation, we have noted clear themes and risks to patient safety in over half (56%) of our inspections. This has resulted in us requesting an immediate improvement plan, which requires practices to tell us within five working days how they will put things right.
The immediate assurance issues included:
- Checks of emergency equipment and drugs not completed on at least a weekly basis. Including instances of missing, expired or not readily accessible items.
- Missing DBS checks, at the appropriate level, for clinical and administrative staff. Including a lack of regular oversight and monitoring by practices.
- Lack of staff immunisation records. Including a lack of capturing and oversight, such as for Hepatitis B.
- Poor compliance with mandatory training, notably safeguarding and to the appropriate level. Including a lack of identified safeguarding leads, clear policies and processes, and effective flagging of vulnerable persons.
- Poor infection, prevention and control (IPC) arrangements. Including expired sterile equipment, poorly cleaned clinical areas, and a lack of IPC audit activity.
The above issues were identified on multiple occasions.
Other immediate assurance issues identified included:
- Medication fridge temperature checks not completed.
- Patient and staff emergency call bells / alarms were not available.
- Patient Group Directions (PGDs) were not dated nor appropriately authorised
- Clinical waste not stored appropriately nor secured.
- Inappropriate storage of controlled drugs.
It is disappointing that many of these findings were identified in the previous year and were highlighted in a past key themes update. It is important that practices, health board primary care teams, and other stakeholders learn from these findings to ensure that patients and staff are protected. Health boards must assure themselves that this learning is effectively shared and implemented to support safe primary care services.
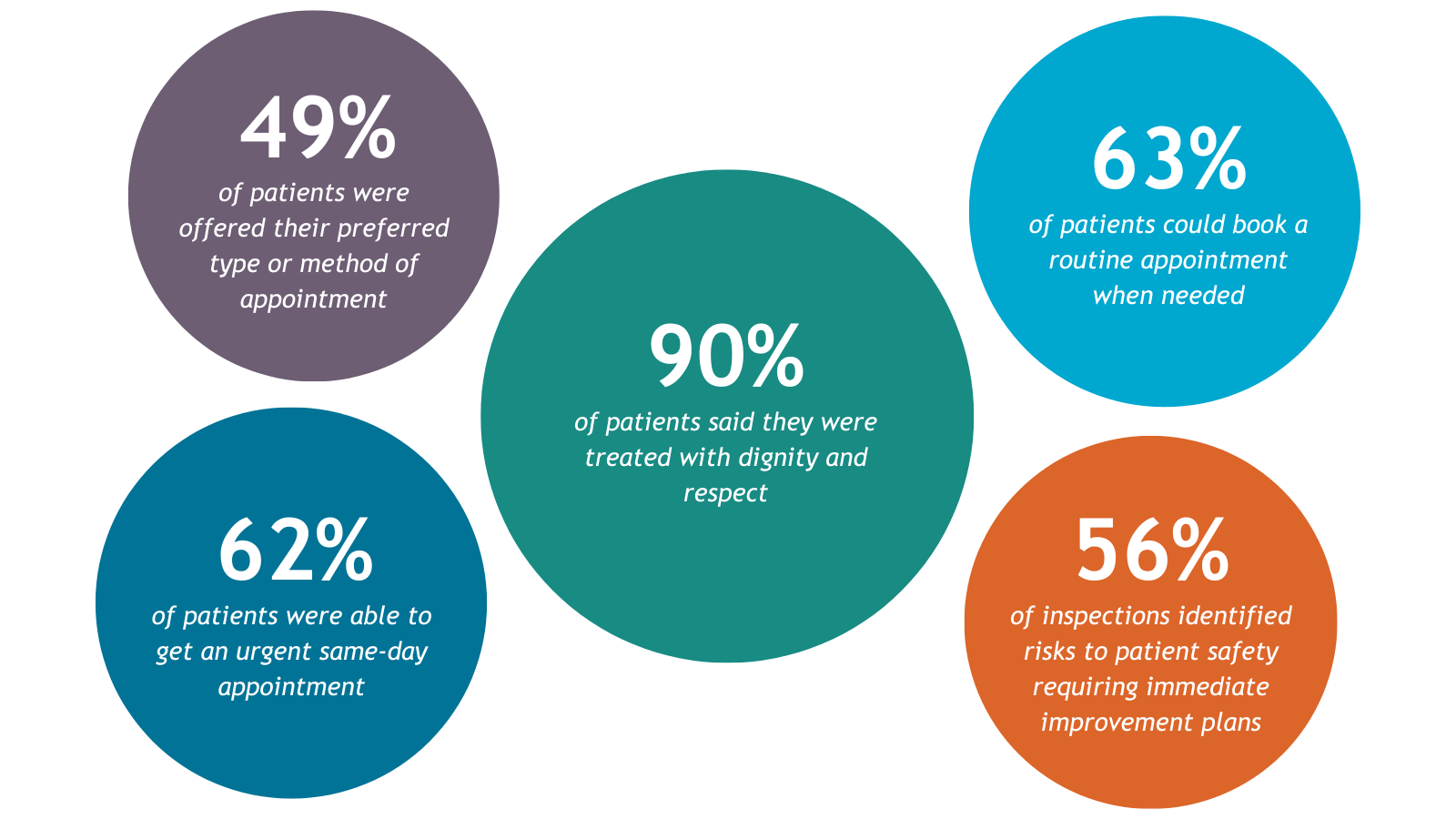
Access to GP services continues to be an area of concern for members of public that we have engaged with. Our GP patient experience surveys for 2024-25, with 650 responses, concluded that over half of patients were able to obtain an urgent same-day appointment (62%) and could book a routine appointment when needed (63%). However, fewer patients told us they were offered their preferred type or method of appointment (49%).
Despite the service pressures, our survey positively concluded that staff continue to treat patients with dignity and respect (90%), with 80% of patients telling us that they felt listened to and involved in decisions about their healthcare.
